Reflections: Global Health Fellowship
Flint strikes steel
 Who knew it would lead to this… Prior to starting my Global Health Fellowship at Dalhousie University, I had no fixed idea what my year would entail. The months of preparation and paperwork gave me a sense of my commitments in Canada, but the specific focus of my fellowship was yet to be determined.
Who knew it would lead to this… Prior to starting my Global Health Fellowship at Dalhousie University, I had no fixed idea what my year would entail. The months of preparation and paperwork gave me a sense of my commitments in Canada, but the specific focus of my fellowship was yet to be determined.
Fortuitously, flint struck steel in the week that I arrived in Halifax. The Chair of the Department of Anaesthesia in Rwanda, Dr Paulin Ruhato was in town. My supervisor, Dr Patty Livingston, Dr Ruhato and I were discussing the plan for my fellowship. A spark of an idea was formed …why not expand on the success of simulation based education in Rwanda and develop a simulation program focusing on the most essential aspects of safe anaesthesia delivery in low-resource settings. This was it!
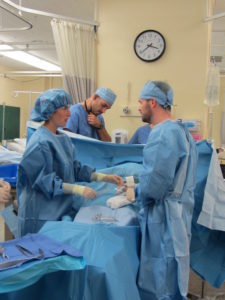 Dr Livingston and I partnered with Dr Christian Mukwesi from the Rwanda Military Hospital to rework and refine this initial idea. We also had to ensure that simulation based education was something that anaesthesia providers in our target audience were receptive to. Through a comprehensive survey, we canvased opinion across anaesthesia providers in Rwanda, enquiring about experience with simulation, thoughts on its utility, interest in a new simulation program, requests for subject matter as well as barriers and enablers for participation. There was an overwhelmingly positive reaction to the idea.
Dr Livingston and I partnered with Dr Christian Mukwesi from the Rwanda Military Hospital to rework and refine this initial idea. We also had to ensure that simulation based education was something that anaesthesia providers in our target audience were receptive to. Through a comprehensive survey, we canvased opinion across anaesthesia providers in Rwanda, enquiring about experience with simulation, thoughts on its utility, interest in a new simulation program, requests for subject matter as well as barriers and enablers for participation. There was an overwhelmingly positive reaction to the idea.
Buoyed by this response, a proposal for the Vital Anaesthesia Simulation Training (VAST) Course was developed; a 3-day simulation based program focusing on both technical and non-technical skills. The case-mix chosen was reflective of common presentations seen at a district hospital in resource-limited settings, focussing on obstetrics, paediatrics, trauma, general surgery as well as neonatal resuscitation, pain and airway management. We strove to develop a program of utility to anaesthesia providers of all levels and that is complimentary to existing programs such as SAFE Obstetrics/Paediatrics, Essential Pain Management, Primary Trauma Care and Helping Babies Breathe. 
Satisfied that the initial workings promoted the ability to deliver safe anaesthesia for the Bellwether procedures as well as reflecting the needs expressed in our survey, we sought further consultation. The course outline was sent for comment to anaesthesia providers in resource-limited settings beyond Rwanda and to experts in the field of global health. Additionally, we collaborated with the team at the Scottish Centre for Simulation and Clinical Human Factors to hone our frameworks for simulation delivery and debriefing.
Various aspects of the course have been ‘tested’ on anaesthesia residents both in Halifax and in Kigali. The pilot of the VAST Course in January will be the maiden run of the course in its entirety. We are also conducting VAST Facilitator courses (train-the-trainer) and are excited for the potential of building a network of Rwandan simulation facilitators. The VAST Course pilot is supported by the Rwanda Society of Anaesthesiologists, the University of Rwanda and the World Federation of Societies of Anaesthesiologists. We are extremely grateful to the Canadian Anesthesiologists’ Society International Education Foundation and Dalhousie University for their financial and logistical support.
In Canada, the final preparations and packing are currently underway for those of us that are travelling to Rwanda. I am extremely excited to transition from course development to delivery. No doubt there will be extensive lessons to be learnt and refinements to me made. The wealth of support and encouragement that has been afforded to me and towards this program has been remarkable. In this moment of reflection, I want to thank everyone who has been involved to help get the VAST Course ready for piloting and I can’t wait to report back on how it goes – December 2017