Reflections on VAST Nyagatare, Rwanda
Dr Patty Livingston’s reflections on VAST Nyagatare, Rwanda (27-29 August 2018)

Nyagatare is a small town in a remote corner of eastern Rwanda, north of Akagera Park, the savannah wildlife reserve. We had arrived at the venue (Nyagatare Diplomat Hotel) the afternoon prior to the course in two jam-packed cars with mannequins, our VAST bins (supplies) and the facilitation team, after driving 100 km of “African massage road” (bumpy and under construction). The massage road followed a somewhat shorter drive on the main highway to reach Rwamagana in the Eastern Province.
Because of geographical isolation, the health care challenges found in low-resource settings are compounded in this region. The VAST Course was designed to bring the benefits of active experiential simulation-based learning – mainstream for health care education in well-resourced settings – to health providers who work with limited resources, often in geographic isolation. Indeed, if the VAST Course can work in Nyagatare, if can probably work anywhere.
 Dr. Christian, the Rwanda VAST Course Director, asked the regional hospital director generals to select 13 local anesthesia providers, nurses and midwives to attend this first of four VAST Courses we are currently offering. The facilitator team included Christian (Rwandan anesthesiologist), Eugene (senior Rwandan anesthesia resident), Laurence (Rwandan simulation centre coordinator), Sara (Canadian research facilitator), Dave (Australian anesthesiologist on a global health fellowship at Dalhousie University), Angela (Canadian anesthesiologist and global health leader) and myself, Patty (Canadian anesthesiologist and longtime friend of Rwanda).
Dr. Christian, the Rwanda VAST Course Director, asked the regional hospital director generals to select 13 local anesthesia providers, nurses and midwives to attend this first of four VAST Courses we are currently offering. The facilitator team included Christian (Rwandan anesthesiologist), Eugene (senior Rwandan anesthesia resident), Laurence (Rwandan simulation centre coordinator), Sara (Canadian research facilitator), Dave (Australian anesthesiologist on a global health fellowship at Dalhousie University), Angela (Canadian anesthesiologist and global health leader) and myself, Patty (Canadian anesthesiologist and longtime friend of Rwanda).
The first morning got off to a rough start. Distances required to travel and heavy rain left us with only one participant arriving on time. We also quickly realized that language would be a far greater challenge than we had experienced during the pilot courses in Kigali. The Nyagatare participants spoke Kinyarwanda and many have limited French or English. Simulation courses depend on communication, so clearly we had a problem. Fortunately, Christian, Eugene and Laurence were able to translate but by lunch we running behind schedule. Additional challenges had to do with noise. A boisterous neighboring shop was playing loud music and there was a political campaign complete with megaphone blasting from the campaign truck. The whole notion of running this course seemed impossible.
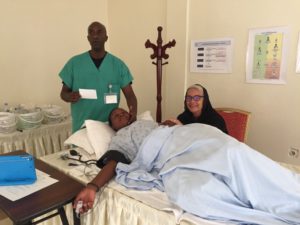 Over lunch on day one, the faculty had an emergency meeting to figure out how to salvage the situation. We decided to repeat the demonstration (faculty-led) scenario to model role-play in simulation. We adapted some of the discussions to include more role-play. The Rwandan facilitators ran debriefings in Kinyarwanda or translated for those of us who spoke English. We spoke slowly. The hotel manager asked the shop to turn down the volume and the political campaign moved on. The participants began to engage in simulation and day one finished on a better note than it had started.
Over lunch on day one, the faculty had an emergency meeting to figure out how to salvage the situation. We decided to repeat the demonstration (faculty-led) scenario to model role-play in simulation. We adapted some of the discussions to include more role-play. The Rwandan facilitators ran debriefings in Kinyarwanda or translated for those of us who spoke English. We spoke slowly. The hotel manager asked the shop to turn down the volume and the political campaign moved on. The participants began to engage in simulation and day one finished on a better note than it had started.
Christian spoke with the participants about punctuality and, happily, days two and three started on time with the full group. The participants became more comfortable with simulation, role-play and debriefing. The VAST Course emphasizes application of non-technical skills in common scenarios found in low-resource settings. We attempted to address content knowledge by using pathology frequent in this context, providing simple preparation reading and asking course participants to answer a set of questions before the course. During the course, key content for scenario performance is provided through interactive discussions before it arises in scenarios. For example, day two is all about obstetric anesthesia care and maternal emergencies. The day starts with group work to answer questions on the medical management of cases that arise the rest of the day in scenarios. We found it worked well for Eugene to use the prepared slides as a guide for himself but to run the case discussion with some demonstration (e.g. how to used left lateral tilt) and use of a flipchart to record answers to questions.
 We continued in this way through days two and three with scenarios, demonstrations, translation and repeating scenarios when needed. Christian led the final course synthesis in Kinyarwanda. The Rwandan facilitators provided feedback that the participants had found the course valuable. One participant said, “I am transformed”. They asked for the course to be repeated often and to include more of their colleagues. Christian said the participants would leave the course as different people.
We continued in this way through days two and three with scenarios, demonstrations, translation and repeating scenarios when needed. Christian led the final course synthesis in Kinyarwanda. The Rwandan facilitators provided feedback that the participants had found the course valuable. One participant said, “I am transformed”. They asked for the course to be repeated often and to include more of their colleagues. Christian said the participants would leave the course as different people.
 The VAST Course in Nyagatare forms part of 4 courses being run consecutively in Rwanda over August / September. An incorporated research project is evaluating VAST’s ability to improve participants’ non-technical skills. The Nyagatare course is also being followed by a facilitator course at the Rwanda Military Hospital, developing Rwandan anaesthesia providers skills in simulation delivery.
The VAST Course in Nyagatare forms part of 4 courses being run consecutively in Rwanda over August / September. An incorporated research project is evaluating VAST’s ability to improve participants’ non-technical skills. The Nyagatare course is also being followed by a facilitator course at the Rwanda Military Hospital, developing Rwandan anaesthesia providers skills in simulation delivery.